USMLE questions don’t reward memorizing drug lists. They reward recognizing which coagulation “lever” is being pulled and
how quickly you can release it. Start with two anchors:
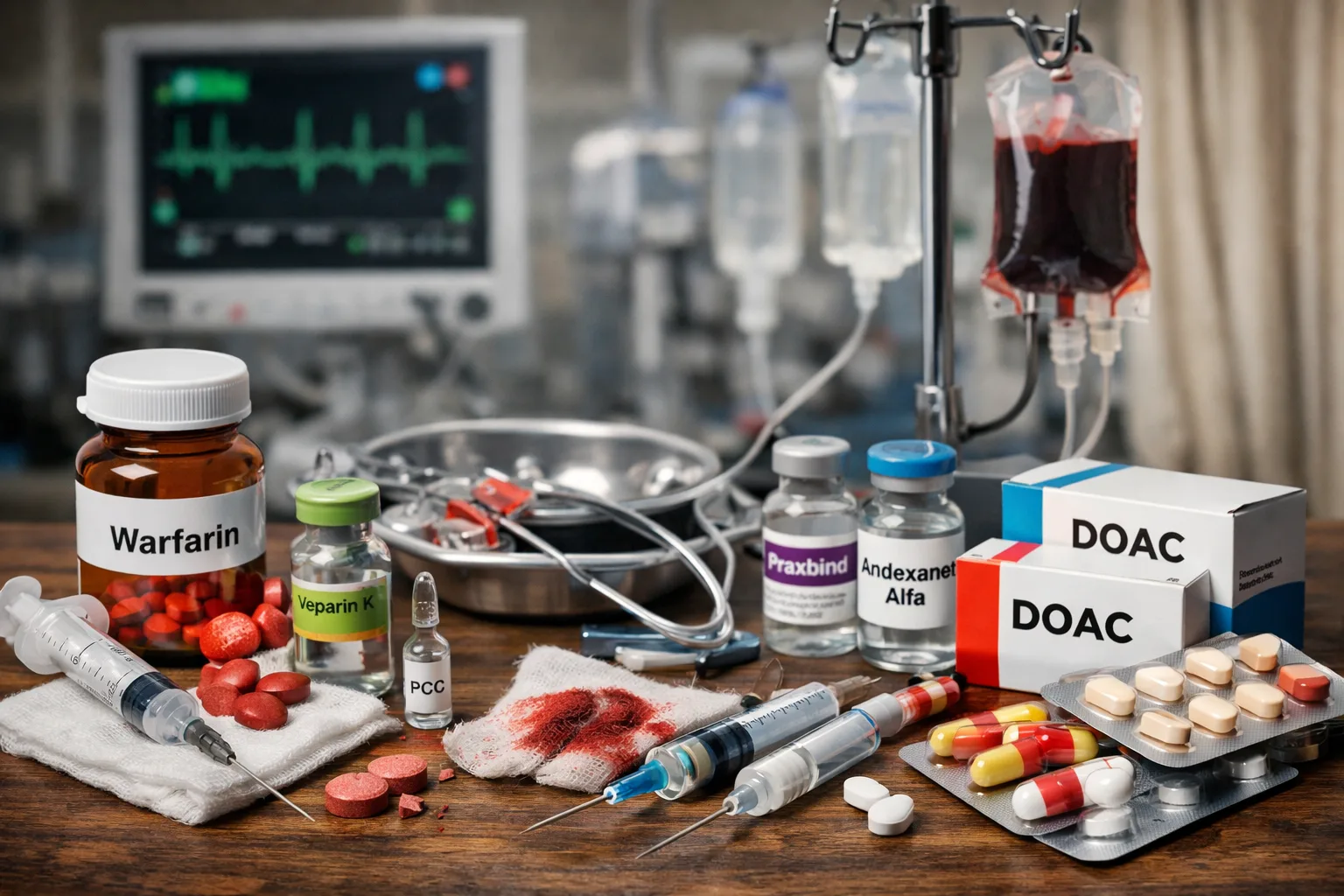
(1) warfarin reduces synthesis of vitamin K–dependent factors (II, VII, IX, X, plus proteins C and S),
and (2) DOACs directly inhibit an activated clotting enzyme (thrombin for dabigatran; factor Xa for
apixaban/rivaroxaban/edoxaban). Everything else—bridging, INR interpretation, and reversal—flows from those anchors.
Warfarin = “slow on, slow off”
- Onset is delayed because existing clotting factors must clear (factor VII falls first; factor II takes longest).
- INR is a lab proxy of factor depletion (especially factor VII), not a direct drug level.
- Early hypercoagulability can occur from protein C depletion—this is why “heparin overlap” exists when starting treatment for acute VTE.
- Practical implication: when you stop warfarin for surgery, you’re waiting for new factors to be synthesized; when you reverse it urgently, you’re replacing factors and giving vitamin K to restart synthesis.
DOACs = “fast on, fast off”
- Predictable kinetics (fixed dosing) and shorter half‑lives in normal renal/hepatic function.
- No routine monitoring for effect in stable patients; standard PT/INR can be misleading.
- Practical implication: for many procedures, you “hold for time” rather than bridge, because anticoagulant effect dissipates quickly.
- In major bleeding, reversal is drug‑specific (idarucizumab for dabigatran; andexanet for certain factor Xa inhibitors), with prothrombin complex concentrate (PCC) as common backup in many pathways.
The exam trick is that the same clinical story (GI bleed, head trauma, urgent surgery) produces different “best next steps” depending on
which anticoagulant is on board, when the last dose was taken, and kidney function. You’ll rarely be asked to calculate a half‑life.
Instead, expect clues like: “last dose this morning,” “creatinine clearance is low,” or “INR is 6.8.” Translate those into one of three
decision lanes:
| Lane |
What the vignette is really testing |
What you do first |
| Bleeding now |
Is it major/life‑threatening? Is there a specific antidote? Can you wait for drug clearance? |
Stabilize (ABCs, transfuse if needed) → stop anticoagulant → targeted reversal when indicated |
| Procedure soon |
Thrombotic risk if you hold? Bleeding risk of the procedure? What’s the minimal interruption time? |
Hold/bridge based on risk category; choose timing based on drug kinetics + renal function |
| Restart question |
When is it safe to resume after hemostasis? What’s the trade‑off between recurrent bleed and thrombosis? |
Restart once bleeding is controlled; earlier for high thrombosis risk, later for high rebleed risk |
Keep these lanes in mind as you work through the next sections. The key is to stop thinking “drug list” and start thinking “mechanism + timing + risk.”
DOAC vs warfarin on test day: choose the drug based on the patient in front of you
USMLE stems often ask you to switch anticoagulants or pick the “most appropriate long‑term therapy.”
A clean way to answer is to sort indications into “DOAC‑friendly” and “warfarin‑preferred,” then apply contraindications.
When DOACs are usually favored (classic exam pattern)
- Nonvalvular atrial fibrillation for stroke prevention (unless a specific exclusion below is present).
- Treatment of DVT/PE in many stable patients after diagnosis (often after brief parenteral anticoagulation depending on agent and setting).
- Patients who struggle with frequent INR checks or variable diet/drug interactions.
When warfarin is often preferred (high‑yield exceptions)
- Mechanical heart valves (DOACs are not used here).
- Moderate–severe mitral stenosis with atrial fibrillation (board‑style “valvular AF”).
- Severe renal impairment may limit DOAC choices; warfarin may be selected when clearance is unreliable.
- Cost/access issues or need for a measurable/adjustable anticoagulant effect.
The exam also loves interaction traps. Warfarin is a pharmacology magnet: antibiotics, amiodarone,
antifungals, and many other drugs can raise INR; leafy‑green intake can lower it; and liver disease or malnutrition can
amplify effect. DOACs have fewer classic food interactions, but absorption and metabolism still matter. When a stem gives you a new medication
and an unexpected bleed, warfarin is the usual culprit unless the question is explicitly targeting a DOAC antidote.
Board-style “which lab matters?” rule
- Warfarin: INR tracks intensity and guides reversal decisions in many vignettes.
- Dabigatran: routine INR is not a reliable measure; specialized tests exist but aren’t usually needed for USMLE decisions.
- Factor Xa inhibitors: PT/INR can be normal even when the drug is active; exam decisions focus on timing of last dose, renal function, and bleed severity.
If you want a practical study tactic: take any anticoagulation question and rewrite it twice—once as warfarin, once as a DOAC—then note how the correct answer changes.
That single exercise trains your “decision lane” thinking faster than memorizing tables.
Bridging made testable: who needs it, who doesn’t, and why
Bridging is a favorite USMLE trap because it looks like “extra safety,” yet in many patients it increases bleeding without meaningfully reducing thrombosis.
Your goal is to identify the small group where interruption is dangerous enough that you temporarily cover them with a short‑acting parenteral anticoagulant
(typically LMWH or IV unfractionated heparin), and to avoid bridging when the underlying drug already has a short offset.
Core principle
Bridging is mainly a warfarin concept. DOACs usually do not require bridging because holding them for a short, procedure‑specific window
clears the anticoagulant effect rapidly in patients with acceptable renal function.
Step-style risk stratification (the way exam writers think)
| Thromboembolism risk if anticoag held |
Examples the test likes to use |
Typical peri-procedure plan |
| High |
Mechanical mitral valve; recent stroke/TIA in AF; VTE within the past few months; severe thrombophilia (e.g., antiphospholipid syndrome)
|
For warfarin: stop in advance and bridge with LMWH/UFH; resume when hemostasis is secure.
For DOACs: usually no bridge; consider specialist input if “extreme risk” scenario appears.
|
| Moderate |
AF with multiple risk factors; remote VTE; bioprosthetic valve with AF |
Individualize; many questions still steer you away from bridging unless the stem emphasizes recent events. |
| Low |
AF without recent stroke; VTE > 12 months ago with no major thrombophilia |
Hold anticoagulant for procedure window; no bridging. |
A testable “mini‑algorithm” for bridging
- Identify the anticoagulant. If it’s a DOAC, default is “no bridge.” If it’s warfarin, continue.
- Identify the reason for anticoagulation. Mechanical valve and recent VTE are the classic “bridge‑leaning” indications.
- Assess procedure bleeding risk. High-bleed procedures force longer interruption; low-bleed procedures may allow minimal hold or even continuation in select scenarios.
- Choose the short‑acting agent if bridging is needed. LMWH for outpatient; IV UFH for very high risk or when rapid on/off is needed.
- Restart thoughtfully. Resume anticoagulation after adequate hemostasis; don’t reflexively restart full-dose the minute the procedure ends if bleeding risk is still high.
USMLE loves to embed bridging inside “med‑surg” logistics: “He’s scheduled for colonoscopy,” “She needs urgent cholecystectomy,” “A spinal procedure is planned.”
Your job is to separate procedure timing from thrombotic urgency. If the patient’s thrombotic risk is low, the safest plan is often simply to hold and restart.
If risk is high, bridging becomes reasonable—but the stem will usually wave a flag like “recent pulmonary embolism” or “mechanical mitral valve.”
NBME-style pitfall: Don’t bridge a DOAC “because it feels safer.” The question writer is often testing that you recognize the short half‑life and choose a timed hold instead.
Score stuck after more questions?
Free reasoning diagnostic
Clinical stems are easier when you can see the decision being tested.
MDSteps helps you separate diagnosis, management, disposition, prevention, counseling, and timing so the next step stops feeling subjective.
Pivot clue isolatedDistractor trap explainedNext study target identified
No credit card required for the free reasoning review. Full access is $27/month after that. Cancel anytime.
Reasoning diagnostic
Still missing questions you thought you understood?
- Find the clue that should have changed your answer
- See why the distractor felt right
- Turn repeated misses into targeted practice
Warfarin reversal: turn “INR panic” into two decisions (bleeding severity + urgency)
Warfarin questions are often framed as an elevated INR. The high-yield move is to avoid treating the number in isolation.
Instead, decide: (1) is there major bleeding or an urgent procedure? and (2) do you need immediate factor replacement?
Vitamin K corrects the deficiency, but it’s not instant. Prothrombin complex concentrate (PCC) replaces factors quickly.
Fresh frozen plasma (FFP) exists, but modern algorithms often favor PCC for rapid reversal because it’s faster and less volume‑heavy.
If INR is high but no bleeding
- Mild elevation: hold/adjust dose; recheck INR (the stem may say “no bleeding, stable”).
- Very high INR: oral vitamin K is often used in many protocols when the number is dangerously high even without bleeding, especially if additional risk factors exist.
- USMLE framing: “supratherapeutic INR found on routine check” is usually managed conservatively unless the number is extreme.
If there is major bleeding or emergency surgery
- Give IV vitamin K (to restart factor synthesis).
- Give 4‑factor PCC (to rapidly replace factors II, VII, IX, X).
- Supportive care: resuscitation, local hemostasis, transfusion as needed.
- USMLE clue: “intracranial hemorrhage on warfarin” almost always points to PCC + IV vitamin K as the reversal backbone.
Why “vitamin K alone” is sometimes wrong
Vitamin K needs the liver to synthesize new factors; it’s corrective but not instantly corrective. In a stable patient without bleeding,
that’s fine. In a crashing patient (massive GI bleed) or a patient with a brain bleed, the exam expects you to restore clotting factors right now.
That’s where PCC earns points: it supplies the factors immediately, while vitamin K prevents “rebound anticoagulation” after PCC wears off.
One-page warfarin reversal flowchart (USMLE logic)
Step 1
Is there major bleeding or urgent surgery?
Step 2
If yes: PCC + IV vitamin K + supportive care.
Step 3
If no: hold warfarin; consider oral vitamin K only when INR is very high or bleeding risk is high.
If you’re using MDSteps to drill this, tag any warfarin item you miss into a “INR + bleeding” deck and force yourself to write the two decisions
(severity + urgency) before looking at the explanation. That single habit usually fixes the entire warfarin reversal category within a week.
Note: exact INR cutoffs vary by protocol; USMLE tends to test the conceptual split between “no bleeding” vs “major bleeding/urgent surgery” rather than fine cut‑points.
DOAC reversal: match the antidote to the drug, then decide if you truly need reversal
DOAC vignettes usually provide (or imply) three details: the specific agent, the timing of the last dose, and kidney function.
The correct answer is rarely “check an INR.” Instead, you decide whether the patient can be managed with supportive care and drug clearance,
or whether they meet criteria for targeted reversal.
| Drug class |
Common agents |
Targeted reversal options (board-relevant) |
| Direct thrombin inhibitor |
Dabigatran |
Idarucizumab for life‑threatening bleeding or urgent procedures; supportive care and time when stable. |
| Factor Xa inhibitors |
Apixaban, rivaroxaban (and sometimes edoxaban) |
Andexanet alfa for major bleeding in select settings; PCC is a common alternative in many institutional pathways. |
When the test wants “supportive care and hold the drug”
- Bleeding is non‑major (hemodynamically stable, controllable source, no critical‑site bleed).
- Last dose was not recent and kidney function is reasonable, so the drug is likely already waning.
- You can achieve hemostasis with local measures (compression, endoscopic control, etc.).
When the test wants “antidote / rapid reversal”
- Life‑threatening hemorrhage (shock, massive transfusion, rapidly expanding bleed).
- Critical-site bleeding (intracranial, spinal, pericardial tamponade—these are “don’t wait” settings).
- Urgent surgery that cannot be delayed long enough for clearance.
USMLE clue: If the stem explicitly names dabigatran and asks “most appropriate reversal agent,” the answer is almost always idarucizumab.
If it names apixaban or rivaroxaban and describes major bleeding, the stem is likely testing andexanet alfa or PCC-based reversal pathways.
Activated charcoal and dialysis: the “rare but testable” details
Two edge tools show up occasionally: activated charcoal if ingestion was very recent (think “just took the dose”),
and hemodialysis for dabigatran in certain scenarios because it has appreciable renal clearance and dialyzability.
Exam writers usually flag this by giving severe renal failure plus dabigatran and ongoing bleeding.
On Step 2, the “antidote” question is often immediately followed by a “restart” question. Don’t stop after you pick the reversal agent—ask yourself what the next move is once bleeding is controlled.
Peri‑procedure holds: the high-yield timing patterns that replace memorization
Peri‑procedure anticoagulation questions feel like a calendar math test, but you can answer most of them with patterns.
The exam is less interested in “exact hours” and more interested in whether you:
(1) appreciate the difference between short‑acting DOACs and long‑offset warfarin, and
(2) understand that procedure bleeding risk and renal function change the hold window.
Warfarin peri‑procedure pattern
- Stop days in advance; INR drifts down as new factors are synthesized.
- Bridge only if thrombotic risk is high (mechanical valve, very recent VTE, etc.).
- Restart after hemostasis; if bridged, the parenteral agent is restarted/continued until INR is therapeutic again.
DOAC peri‑procedure pattern
- Hold based on bleeding risk of the procedure and renal function.
- Low bleed risk procedures often need only a short hold (or sometimes none, depending on the setting).
- High bleed risk procedures and impaired renal clearance require a longer hold window.
- Bridging is generally unnecessary.
A “procedure risk” shortcut that matches USMLE stems
- Low bleed risk: superficial dermatologic procedures, many dental procedures, some endoscopy without high‑risk interventions.
- High bleed risk / neuraxial: major surgery, organ biopsies, spinal/epidural anesthesia—these get longer holds and more cautious restarts.
Common “hold vs bridge” vignette conversions
| Stem detail |
What it means |
Likely best action |
| Elective colonoscopy; AF; no recent stroke |
Low–moderate thrombotic risk |
Hold anticoagulant appropriately; no bridge |
| Mechanical mitral valve; elective surgery |
High thrombotic risk |
Stop warfarin and bridge with LMWH/UFH |
| Apixaban; normal renal function; minor procedure |
Short offset, low bleed risk |
Short hold or timed scheduling; no bridge |
| Dabigatran; CKD; high‑bleed surgery |
Prolonged effect with renal impairment |
Longer hold; consider antidote if truly urgent |
A practical study move is to memorize relationships, not times: “higher bleed risk = longer hold,” “worse kidneys = longer hold,” and “warfarin = bridge only for high thrombosis risk.”
Those three rules answer most Step‑style peri‑procedure questions.
Restarting anticoagulation after bleeding: the “re-bleed vs clot” trade that USMLE tests
Restart questions are about clinical reasoning, not courage. The test wants you to weigh thrombotic risk if off anticoagulation
against rebleeding risk if restarted too soon. The stem often provides a bleeding site (GI vs intracranial),
hemostasis status (endoscopic control vs ongoing oozing), and the underlying indication for anticoagulation (AF vs recent PE vs mechanical valve).
Factors pushing earlier restart
- Mechanical valve or very high cardioembolic risk
- Recent VTE or ongoing provoking factor
- Bleeding source controlled with high confidence (definitive endoscopic therapy, surgical hemostasis)
Factors pushing later restart
- Intracranial or critical-site bleed with high rebleed morbidity
- Unclear bleeding source or incomplete hemostasis
- Severe uncontrolled hypertension or concurrent antiplatelet therapy raising bleed risk
Board-style “restart” phrasing and what it means
- “After endoscopic hemostasis, when should anticoagulation be resumed?” → resume once stable; earlier if thrombosis risk is high.
- “Patient had intracerebral hemorrhage on anticoagulation; next step?” → stop and reverse acutely; later decisions are individualized and depend on indication and neurologic stability.
- “He’s now stable; what prophylaxis should he receive while off full anticoagulation?” → mechanical prophylaxis or low-dose pharmacologic prophylaxis when safe (depending on the stem’s bleeding control).
Test-taker move: If you’re unsure, choose the answer that explicitly states bleeding control first (e.g., “confirm hemostasis”),
then safe resumption based on risk. USMLE punishes “restart immediately” answers unless the stem screams extreme thrombosis risk and controlled bleeding.
Rapid-Review Checklist (bookmark this for dedicated blocks)
- Always classify bleeding: major vs non-major vs critical-site.
- Warfarin + major bleed: PCC + IV vitamin K.
- Dabigatran + major bleed: idarucizumab.
- Apixaban/rivaroxaban + major bleed: andexanet (select) or PCC pathway.
- Bridging: mostly a warfarin question; DOACs usually “hold by time.”
- Restart: earlier for high clot risk, later for high rebleed risk; always after hemostasis.
Exam-Day Essentials
- Circle the anticoagulant in the stem.
- Underline “last dose” timing and kidney function.
- Decide your lane: bleeding now, procedure soon, or restart.
- Pick the simplest safe action that matches the lane.
- After choosing, ask “what would I do next?” to catch two-step questions.
If you’re building an error log, MDSteps’ automatic flashcard decks from misses work best here: create one card per “lane” and force yourself to write a one‑sentence justification before flipping to the answer.
Practice with vignette templates: the fastest way to stop missing anticoagulation questions
The quickest path to mastery is not rereading guidelines—it’s rehearsing templates. Below are five classic stems that repeatedly appear on Step 1 and Step 2 CK.
Work them until your response is automatic, then mix them by swapping the anticoagulant and changing kidney function.
Stem: Elderly patient falls, CT shows intracranial hemorrhage, taking an anticoagulant.
What the test wants: Stabilize, stop the drug, and choose rapid reversal based on the specific agent (warfarin → PCC + IV vitamin K; dabigatran → idarucizumab; factor Xa inhibitor → andexanet/PCC pathway). Critical-site bleeding is the key signal.
Stem: Patient on warfarin, INR elevated, no bleeding.
What the test wants: Hold/adjust warfarin; consider vitamin K only when the INR is extremely high or bleeding risk is significant. The “gotcha” is avoiding aggressive reversal when there is no bleeding and no urgent procedure.
Stem: Needs emergent operation; on anticoagulant; last dose was recent.
What the test wants: If surgery can’t wait, choose rapid reversal matched to drug; if it can wait, hold and allow clearance (especially for DOACs). Timing language (“in 2 hours,” “tomorrow morning”) is your biggest clue.
Stem: Elective procedure scheduled; on warfarin or DOAC; asks about bridging.
What the test wants: Warfarin may need bridging only for high thrombotic risk. DOACs are typically held for a procedure-specific window without bridging. Renal impairment extends DOAC hold time.
Stem: Bleeding controlled; asks when and what to restart.
What the test wants: Restart after hemostasis, balancing clot risk vs rebleed risk. The exam usually rewards a plan that acknowledges stability first and prioritizes high thrombotic risk conditions for earlier resumption.
How to drill this in 20 minutes
- Do 10 mixed anticoagulation questions timed.
- For every miss, rewrite the stem into your three lanes (bleeding, procedure, restart).
- Make one flashcard: “If X drug + Y scenario → Z first action.”
- Repeat in 48 hours; you should see rapid convergence.
Medically reviewed by: R. Patel, MD (Internal Medicine)