The “one-table” framework: stop guessing, start sorting
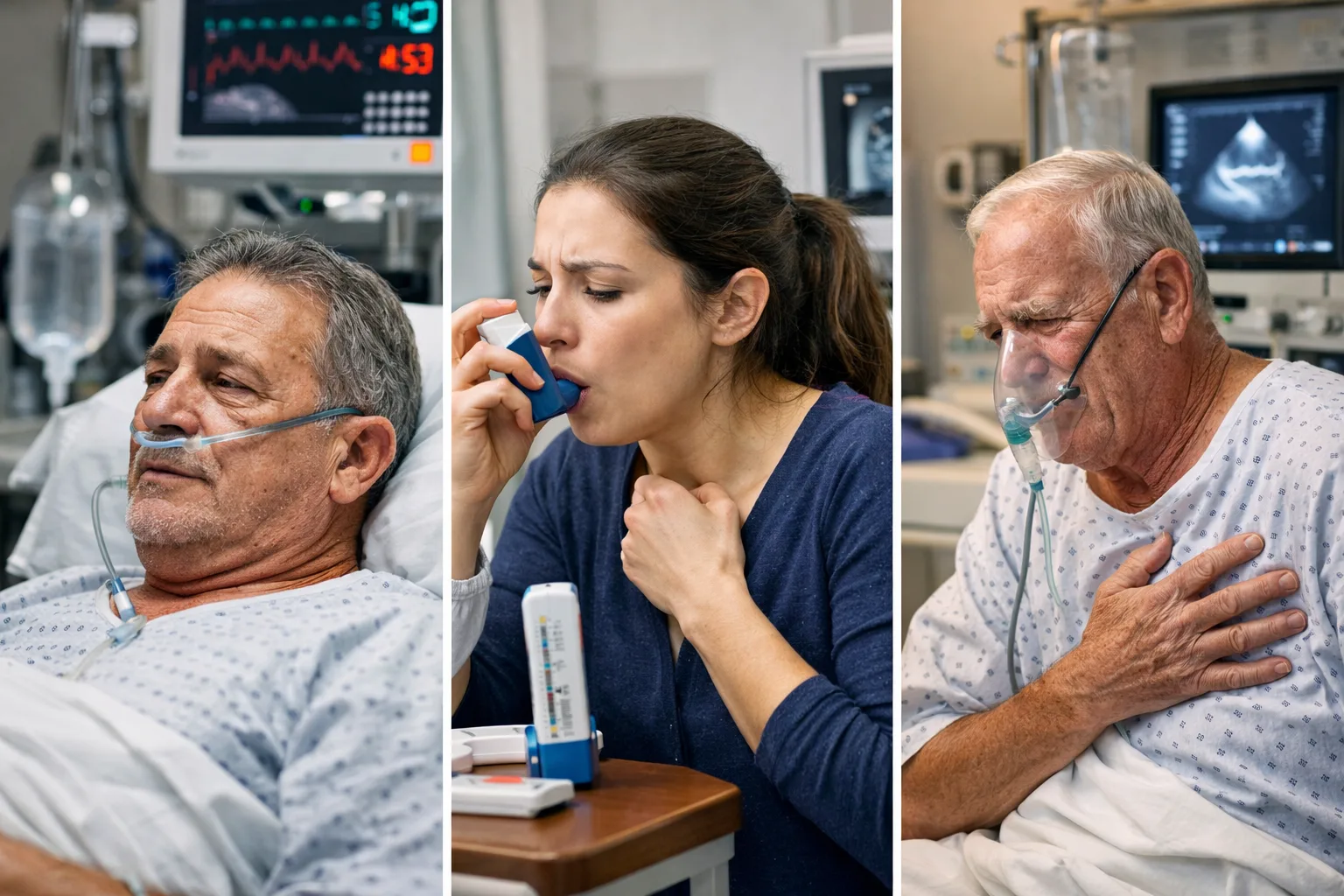
Every USMLE season, the same vignette shows up with different costumes: a patient is short of breath, wheezing, and “looks uncomfortable.”
The stem gives you just enough data to tempt a reflex diagnosis, then the question asks for the next best step.
Your job is not to memorize three separate diseases. Your job is to sort the presentation into one of three buckets:
obstructive airway (asthma), chronic obstructive airway with exacerbation (COPD flare), or volume/pressure overload (acute decompensated heart failure).
Here’s the key USMLE reality: vignettes rarely give you every test. They give you a few “anchor” clues and then hide the rest behind distractors.
So your strategy needs to be robust to missing data. The most reliable approach is to build a mental table with four columns:
time course, bedside pattern, objective tests you can trust, and treat-first moves.
If you can fill those four columns, you can answer 80% of questions even before imaging returns.
The Differentiation Table (high-yield, exam-ready)
| Feature |
Asthma exacerbation |
COPD exacerbation |
CHF exacerbation (acute HF) |
| Typical patient |
Often younger, atopy/eczema/allergic rhinitis, variable symptoms |
Older, smoking/biomass exposure, chronic cough/sputum, baseline dyspnea |
Older, CAD/HTN/valvular disease, prior HF, volume triggers |
| Time course |
Minutes–hours; episodic; often after trigger (allergen, viral) |
Hours–days; often infectious trigger; “worse than baseline” |
Hours–days; after salt load, missed diuretics, ischemia, arrhythmia |
| Symptoms |
Chest tightness, cough, nocturnal/early morning symptoms |
Increased dyspnea, sputum volume/purulence, cough |
Orthopnea, PND, weight gain, leg edema, abdominal distension |
| Breath sounds |
Diffuse wheeze; may be “silent chest” if severe |
Wheeze + prolonged expiration; often diminished sounds |
Crackles/rales, possible wheeze (“cardiac asthma”), S3 |
| Work of breathing |
Accessory muscle use; pulsus paradoxus in severe cases |
Pursed-lip breathing; tripod; barrel chest (baseline) |
Tachypnea; may have frothy sputum in pulmonary edema |
| Oxygen/CO2 |
Hypoxemia; early low CO2 (hyperventilation), later rising CO2 = fatigue |
Baseline higher CO2; worsening hypercapnia common |
Hypoxemia; CO2 usually normal/low unless severe fatigue/other lung disease |
| Chest X-ray |
Often normal or hyperinflation; no cardiomegaly |
Hyperinflation/flattened diaphragms; may show pneumonia |
Cardiomegaly, vascular congestion, interstitial/alveolar edema, pleural effusions |
| BNP/NT-proBNP |
Usually not elevated |
May be mildly elevated if strain/comorbidity; interpret with context |
Often elevated; low value argues against HF (watch obesity and renal disease) |
| Response to bronchodilator |
Often dramatic, rapid improvement |
Partial improvement; baseline limitation remains |
Minimal unless concomitant bronchospasm |
| Treat-first moves |
Inhaled SABA ± ipratropium, systemic steroids, O2 as needed |
SABA + anticholinergic, systemic steroids, antibiotics if indicated; consider NIV |
Loop diuretic, nitrates (if hypertensive), oxygen/ventilation support; treat trigger |
| Classic USMLE trap |
Normal CXR doesn’t rule out severe asthma; rising CO2 is bad |
Over-oxygenation fear vs under-treating hypoxemia; missing pneumonia |
“Wheezing” misleads—look for orthopnea, edema, CXR congestion |
Use this table as a sorting key: time course + volume clues + CXR pattern + objective gas exchange trends beat any single symptom.
Notice what the table does not do. It doesn’t pretend that wheeze is exclusive to airway disease.
It doesn’t rely on “smoker = COPD” as a single deciding rule. And it doesn’t assume you’ll be given an echocardiogram.
Instead, it elevates clues the USMLE loves: orthopnea/PND, cardiomegaly/edema on CXR,
sputum change, and CO2 trajectory.
Exam mindset: Always ask, “What kills first?” In asthma/COPD, it’s ventilatory failure and fatigue.
In acute HF, it’s hypoxemia from pulmonary edema and hemodynamic collapse. Your next step should protect the immediate threat.
History that separates the three in 30 seconds
On test day, you rarely have time to “work up dyspnea” like a full clinic visit. The stem gives you a snapshot.
Your goal is to harvest discriminating history—details that shift pretest probability enough to choose management.
A useful rule: if the question stem includes volume language (weight gain, swelling, orthopnea), trust it.
If it includes airway variability (episodic symptoms, triggers, nocturnal cough), trust that.
If it includes baseline chronicity (daily sputum, long smoking history, chronic exertional limitation), lean COPD.
Asthma: “variable and triggered”
- Symptoms vary day-to-day and within the day
- Triggers: allergens, exercise, cold air, viral infection
- Atopy clues: eczema, allergic rhinitis, family history
- Nocturnal/early-morning cough or wheeze
- Prior dramatic response to inhaler is a big tell
COPD flare: “worse than baseline”
- Older + exposure history (smoking, biomass, occupational)
- Chronic productive cough; “morning sputum” pattern
- Now: increased dyspnea, sputum volume/purulence
- Frequent prior exacerbations or home O2
- Infectious prodrome (URI) is common
Acute HF: “lying flat is the problem”
- Orthopnea: needs extra pillows to sleep
- Paroxysmal nocturnal dyspnea (PND)
- Weight gain, edema, abdominal fullness
- Medication nonadherence, NSAIDs, salt load
- New AF, ischemia, hypertensive urgency
USMLE writers often hide the best history clue in a single phrase. Examples:
“He sleeps in a recliner” is orthopnea until proven otherwise. “His inhaler worked great last time” screams reversible bronchospasm.
“His sputum turned green” is not a microbiology puzzle—it’s a COPD exacerbation clue that will change antibiotic choice.
Another classic move is medication context. A patient “on a daily inhaled corticosteroid and long-acting bronchodilator” with flare symptoms
sounds like asthma or overlap; a patient “who ran out of furosemide” points to HF decompensation; a patient “using oxygen at home” suggests advanced COPD.
Don’t overread medication lists, but do use them as priors.
Quick stem translator
| Stem phrase |
Likely meaning |
Bucket it favors |
| “Wakes up gasping at night” |
PND / pulmonary congestion episodes |
Acute HF |
| “Wheezing but also swelling” |
Cardiac asthma or mixed pathology |
HF first, then reassess |
| “Green sputum” |
Increased purulence (bacterial trigger more likely) |
COPD flare |
| “Symptoms vary with seasons/pets” |
Allergic trigger / variable airflow limitation |
Asthma |
| “Can’t catch breath after missing meds” |
Nonadherence trigger (diuretics, beta-blocker, etc.) |
Acute HF (common) |
Bedside exam & vitals: where USMLE points hide
The physical exam is not a nostalgia exercise. On USMLE, it’s a scoring system:
the exam finds the few bedside findings that reliably correlate with physiology and expects you to use them.
For this triad, the highest-yield exam skills are (1) assessing volume status,
(2) recognizing severe bronchospasm vs “noisy but stable,” and (3) reading vital sign context without overreacting.
Volume status checklist (HF favored if multiple positive)
- Elevated JVP (especially with hepatojugular reflux)
- Peripheral edema, ascites, hepatomegaly
- S3 gallop (volume overload / reduced compliance)
- Basilar crackles that do not clear with cough
- Cold extremities, narrow pulse pressure (poor perfusion)
Danger signs in obstructive flares (asthma/COPD)
- “Silent chest” (very little air movement) = impending failure
- Altered mental status, fatigue, inability to speak full sentences
- Rising PaCO2 or normalizing CO2 after initial low (bad trend)
- Accessory muscle use + paradoxical abdominal motion
- Hypotension from dynamic hyperinflation (severe air trapping)
A frequent NBME trick is giving you a patient with wheeze and tachycardia, then asking for the “most likely cause of symptoms.”
Tachycardia is nonspecific: anxiety, hypoxemia, beta-agonists, fever, pain. Don’t let it dominate your reasoning.
Instead, look for positional dyspnea (worse lying down), signs of congestion, and objective oxygenation trends.
Another trap is assuming crackles automatically mean HF. COPD patients can have crackles from pneumonia, atelectasis, or fibrosis.
Asthma patients can have minimal crackles and still be critical (airflow obstruction is the problem, not fluid).
The best single exam differentiator is often orthopnea + edema + cardiomegaly as a cluster rather than any isolated finding.
Board-style nuance: “Cardiac asthma” is real test language: pulmonary edema can cause wheeze.
If the stem hints at congestion (orthopnea, edema, cardiomegaly), treat HF physiology first, then reassess airway response.
Finally, think about blood pressure phenotype in acute HF. A hypertensive patient with flash pulmonary edema often improves quickly with nitrates and diuresis,
while hypotension suggests cardiogenic shock physiology where pressors/inotropes and careful ventilation strategy become the priority.
The USMLE won’t ask you to run an ICU, but it will ask you to pick the correct “next best step” when a patient is clearly unstable.
Score stuck after more questions?
Free reasoning diagnostic
Clinical stems are easier when you can see the decision being tested.
MDSteps helps you separate diagnosis, management, disposition, prevention, counseling, and timing so the next step stops feeling subjective.
Pivot clue isolatedDistractor trap explainedNext study target identified
No credit card required for the free reasoning review. Full access is $27/month after that. Cancel anytime.
Reasoning diagnostic
Still missing questions you thought you understood?
- Find the clue that should have changed your answer
- See why the distractor felt right
- Turn repeated misses into targeted practice
Objective tests: ABG patterns, CXR traps, and BNP interpretation
When a question gives you labs or imaging, it’s not to pad word count. It’s to test whether you can interpret physiology.
For differentiating obstructive flares from acute HF, the most board-relevant tests are:
arterial/venous blood gases, basic metabolic panel, chest radiograph, and natriuretic peptides.
You don’t need every number; you need the pattern and the direction of change.
ABG/VBG: the CO2 story is the story
In asthma, early exacerbations typically cause hyperventilation and low PaCO2 (respiratory alkalosis).
A key red flag is a PaCO2 that rises toward normal or becomes elevated—this suggests fatigue and impending ventilatory failure.
In COPD, chronic CO2 retention can exist at baseline; an exacerbation often pushes CO2 higher with worsening acidosis.
In acute HF, CO2 is usually normal or low due to tachypnea, unless the patient is tiring or has overlapping lung disease.
Pattern table: gases & chemistry
| Test pattern |
What it suggests |
Common USMLE pitfall |
| Low CO2 in asthma → later normal/high CO2 |
Fatigue/impending respiratory failure |
Thinking “normal CO2 = improving” |
| Chronic elevated HCO3− + high CO2 |
Chronic COPD compensation |
Calling it acute metabolic alkalosis |
| Metabolic alkalosis + hypokalemia |
Diuretic effect (HF meds) or vomiting |
Ignoring that the “trigger” is medication-related |
| Hypoxemia with relatively normal CO2 |
V/Q mismatch (pneumonia, HF edema, PE) |
Assuming it must be asthma/COPD |
CXR: don’t overcall, don’t undercall
The chest X-ray is one of the most efficient discriminators because it “sees” congestion and cardiomegaly.
But it’s also a trap: a normal CXR does not rule out a severe asthma attack, and hyperinflation can coexist with HF.
Look for the pattern: cardiomegaly + vascular congestion + Kerley B lines + pleural effusions points toward HF physiology;
hyperinflation with flattened diaphragms points toward COPD; a focal infiltrate suggests pneumonia as a trigger.
BNP/NT-proBNP: what boards want you to know
Natriuretic peptides are high-yield because they help with uncertainty. USMLE doesn’t need you to memorize every cutoff,
but it expects you to know the logic: low peptide levels make HF less likely; higher levels support HF in the right context.
The nuance is in false positives and false negatives. Renal dysfunction can elevate values; obesity can lower them.
COPD with right-heart strain can mildly increase them. So treat BNP like a “vote,” not a verdict.
Practical takeaway: If the stem gives you a low natriuretic peptide plus a clear obstructive picture, HF falls down your list.
If it gives you a high value plus congestion signs on imaging/exam, HF rises quickly.
Spirometry logic (and why you rarely need it during an acute stem)
Spirometry is how you confirm obstructive disease in real life, but on USMLE it shows up selectively.
In acute presentations, you often treat first and confirm later. Still, you need a working understanding of what spirometry patterns mean,
because a question may include pre- and post-bronchodilator values as the “one clean clue” to distinguish asthma from COPD.
Start with basics: obstruction is a reduced FEV1/FVC ratio. Asthma is characterized by variable airflow limitation—often reversible.
COPD is characterized by persistent airflow limitation—less reversible, and usually progressive.
The exam-friendly interpretation: if bronchodilator response produces a large improvement in FEV1 and symptoms,
asthma becomes more likely. If the ratio remains low with limited reversibility and the patient has exposure history, COPD becomes more likely.
Overlap exists, but boards mostly test the canonical patterns.
How USMLE uses spirometry in questions
- Confirming the diagnosis: “Variable airflow limitation” supports asthma; “persistent obstruction” supports COPD.
- Testing inhaler selection: persistent symptoms in asthma → controller therapy emphasis; COPD → bronchodilator strategy emphasis.
- Building differential: dyspnea with normal spirometry pushes you toward HF, anemia, PE, or deconditioning.
Here’s the non-obvious high-yield point: spirometry can be normal between asthma attacks.
That’s why guidelines emphasize documenting variable symptoms plus objective variability over time.
In contrast, COPD spirometry tends to stay abnormal because airflow limitation is persistent.
If you see “normal spirometry today, abnormal last month,” think asthma variability.
If you see “longstanding obstruction,” think COPD.
What about HF? Spirometry is not a first-line HF test, but pulmonary congestion can transiently reduce lung volumes and cause dyspnea without classic obstruction.
That’s why a dyspneic patient with normal obstruction indices and strong volume clues should not be labeled “asthma” simply because they wheeze.
Again: wheeze is a sound; the diagnosis is physiology.
Test-taking hack: In acute stems, choose the intervention that prevents deterioration first (oxygenation/ventilation/hemodynamics).
Spirometry is usually a “later” diagnostic confirmatory tool unless the question explicitly hands it to you.
Treat-first algorithms: what to do before you have “perfect certainty”
USMLE management questions reward safe, physiology-aligned decisions. That means you often start treatment while you refine the diagnosis.
The key is to choose interventions that help the likely disease and do not significantly harm the alternatives.
Below is a practical bedside algorithm you can apply to most vignettes.
Decision flow (text-based, board-ready)
Step 1: Stabilize
- Assess airway, breathing, circulation
- Pulse ox; supplemental O2 if needed
- Consider NIV if severe distress/hypercapnia
Step 2: Split by congestion clues
- Orthopnea/PND? edema? JVP?
- CXR cardiomegaly/edema?
- High BNP supports HF in context
Step 3: Treat targeted physiology
- Obstructive: bronchodilators + steroids
- COPD flare: add antibiotics when indicated
- HF: diuresis ± nitrates; fix trigger
This mirrors USMLE logic: stabilize first, then choose the most physiology-aligned next action based on discriminating clues.
Asthma exacerbation: the core moves
Boards expect you to recognize rapid-acting bronchodilation plus systemic anti-inflammatory therapy.
Inhaled short-acting beta agonist (SABA) is first-line; adding inhaled anticholinergic can help in moderate/severe attacks.
Systemic corticosteroids reduce relapse and speed recovery. Oxygen is supportive; titrate to adequate saturation.
If you’re given “silent chest,” rising CO2, or exhaustion, the question is about impending failure, and ventilatory support becomes the next step.
COPD exacerbation: same lane, extra branches
COPD flares share bronchodilators and systemic steroids, but add two high-yield branches:
(1) noninvasive ventilation in hypercapnic respiratory failure to reduce intubation risk, and
(2) antibiotics when bacterial features are present (classically increased dyspnea, sputum volume, and sputum purulence).
The test won’t force you to memorize every antibiotic regimen, but it will test that you recognize when antibiotics are indicated.
Per guideline logic, the goal is to minimize the current flare impact and prevent early recurrence.
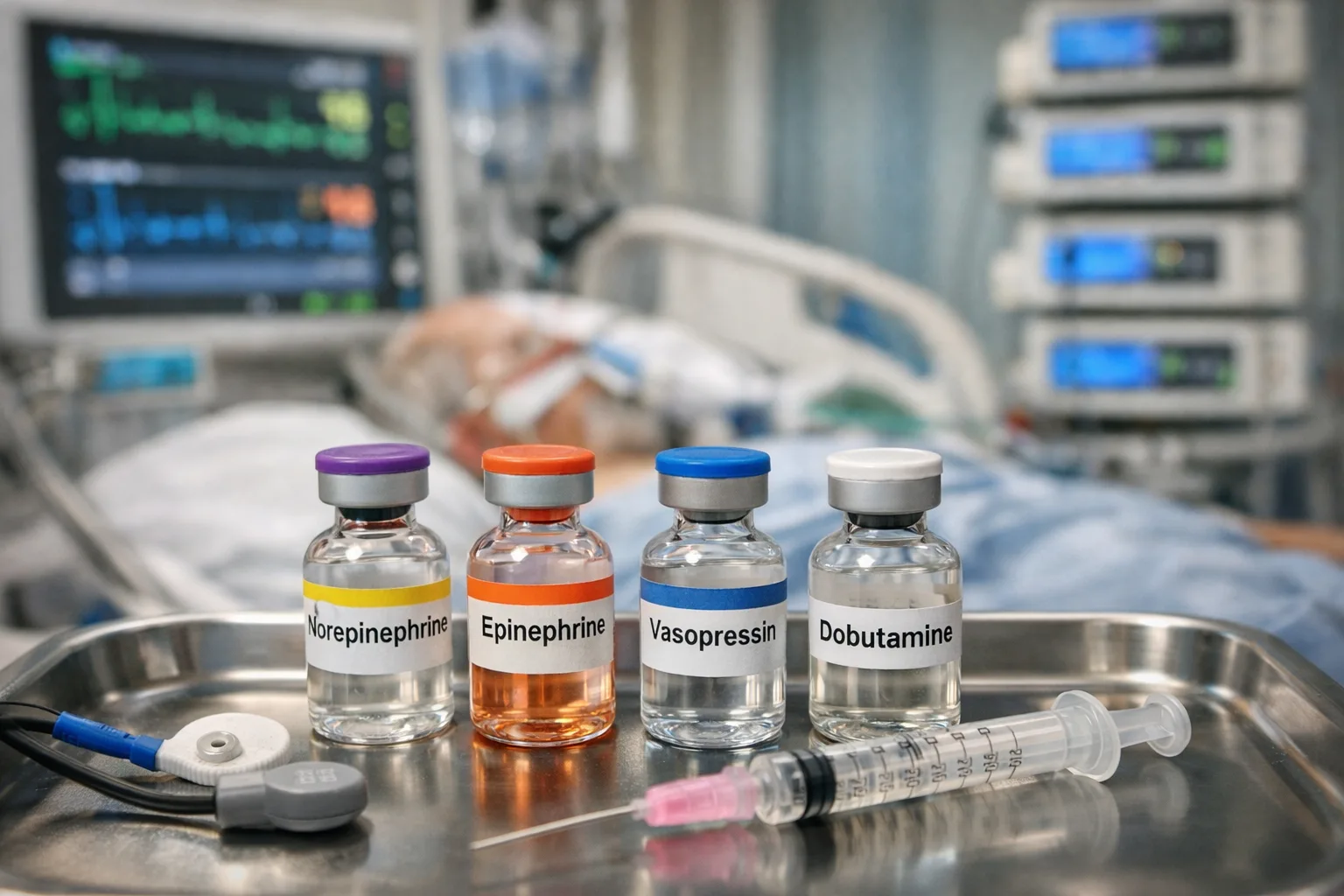
Acute HF: treat congestion (and the trigger)
Acute decompensated HF treatment is about unloading the lungs and supporting perfusion.
Loop diuretics are foundational for volume overload. In hypertensive pulmonary edema, vasodilators (like nitrates) can rapidly improve symptoms.
If the stem suggests ischemia, arrhythmia, or infection, treat the precipitant in parallel.
And remember: wheeze does not exclude HF—if congestion is present, bronchodilators alone won’t solve the problem.
What’s safest when you’re unsure?
- Oxygen (titrate to appropriate saturation) is generally safe across all three.
- NIV can help both hypercapnic COPD flares and HF pulmonary edema when used appropriately.
- Bronchodilator trial is reasonable if wheeze is prominent and there’s no clear contraindication.
- Diuresis is helpful if congestion is convincing; avoid reflex diuresis in clear dehydration/sepsis.
Overlap, traps, and “mixed pictures”: how exam writers punish shortcuts
Real patients do not read textbooks, and neither do USMLE question writers. The easiest way to lose points is to rely on single-feature shortcuts:
“Wheeze equals asthma,” “Smoker equals COPD,” “Crackles equals HF.” Mixed physiology is common:
COPD patients develop HF, HF patients wheeze, asthma patients get pneumonia. Your goal is not to label perfectly; it’s to choose
the safest, most effective next step based on the dominant physiology and the immediate risk.
Trap 1: “Cardiac asthma” masquerading as obstructive disease
If the stem includes orthopnea, PND, edema, and cardiomegaly, that cluster should outweigh wheeze.
Acute pulmonary edema can cause bronchial mucosal edema and airway narrowing, producing wheeze.
The correct answer often involves diuretics and vasodilators rather than escalating bronchodilators.
A bronchodilator may be given as a trial, but it shouldn’t replace treating congestion.
Trap 2: Infection triggers everything
Viral URIs commonly trigger asthma and COPD flares. Bacterial pneumonia can trigger HF decompensation by increasing metabolic demand and causing hypoxemia.
If the CXR shows a focal infiltrate plus fever and leukocytosis, your next step may involve antibiotics even if the patient wheezes.
Don’t let a single disease label blind you to the trigger.
Trap 3: CO2 “normalization” in asthma
This one is classic. An anxious asthmatic hyperventilates early and blows off CO2. If you see a PaCO2 that is “normal” in a sick-looking patient,
that can be a sign they are tiring and can no longer hyperventilate. This is when the vignette pivots to ventilatory support decisions.
Many students miss it because they interpret “normal” as reassuring.
Trap 4: Beta-blocker fear vs HF benefit
A test item may mention a patient with COPD and HF and ask about medication choices.
The board-relevant concept is that cardioselective beta-blockers can still be used in many patients with obstructive lung disease when indicated for HF/CAD,
but acute bronchospasm episodes require caution. If the question is about acute dyspnea management, you prioritize stabilization first; if it’s chronic therapy,
you weigh risk/benefit and the clinical context rather than using absolute prohibitions.
When two diagnoses are plausible, use this tie-breaker
| Tie situation |
Best next discriminator |
Immediate “safe” action |
| Wheeze + edema |
CXR for congestion/cardiomegaly; natriuretic peptide |
O2 + consider NIV; start diuresis if congestion convincing |
| Smoker + variable symptoms |
Bronchodilator response history/spirometry pattern |
SABA trial + systemic steroids if moderate/severe flare |
| Dyspnea + fever |
CXR infiltrate; sputum change; WBC trend |
O2 + treat infection trigger in parallel |
| Hypercapnia + “wet” lungs |
Baseline COPD history vs new congestion pattern |
NIV while sorting; avoid delays in escalation if tiring |
If you want to drill these mixed-picture stems efficiently, use a system that forces you to label the dominant physiology before you read answer choices.
On the MDSteps platform, our Adaptive QBank (16,000+ questions) lets you tag misses as “airway vs volume vs mixed” and then auto-build a review set and flashcards from those misses,
which is one of the fastest ways to eliminate these recurring traps.
Rapid-Review Checklist: the exam-day differentiator
On exam day, you don’t need a perfect diagnosis—you need a defensible, physiology-based next step.
Use this checklist to move fast and avoid the common traps.
Rapid sort (10-second screen)
- Orthopnea/PND + edema → HF rises
- Variable triggers + atopy → asthma rises
- Chronic sputum + exposure + baseline limitation → COPD rises
- Focal infiltrate + fever → infection trigger (don’t ignore)
Red flags (act before you “finish the workup”)
- Silent chest, exhaustion, altered mental status
- Rising CO2 with distress (especially in asthma)
- Hypotension + pulmonary edema signs
- Severe hypoxemia despite oxygen
Answer-choice pattern recognition
| What the question is really testing |
Clue in the stem |
Answers you should expect |
| Need ventilatory support |
Fatigue, rising CO2, inability to speak, AMS |
NIV, intubation/ventilation strategy, ICU escalation |
| Need bronchodilation + anti-inflammatory therapy |
Diffuse wheeze, triggers, rapid onset, no congestion signs |
SABA, ipratropium, systemic steroids |
| Need diuresis/vasodilation |
Orthopnea, edema, cardiomegaly, congestion on CXR |
Loop diuretic, nitrates (if hypertensive), treat trigger |
| Need antibiotics (trigger management) |
Purulent sputum, infiltrate, fever, systemic signs |
Antibiotics alongside core flare therapy |
If you’re building a study plan, use this topic as a high-yield “integrator” across Steps:
Step 1 focuses on mechanism (bronchoconstriction, inflammation, ventilation-perfusion).
Step 2 CK focuses on next-step diagnosis and management.
Step 3 emphasizes disposition, escalation, and comorbidity overlap.
A smart schedule: one day of concept review + two short QBank blocks + one day later for mixed stems.
Your goal is not to memorize more facts; it’s to become faster at sorting physiology.
Final exam-day rule: When you’re torn between “airway” and “volume,” trust congestion clusters (orthopnea/edema/cardiomegaly)
and CO2 trajectory. Treat the life threat first, then reassess the response.
Medically reviewed by: Andrea Patel, MD (Internal Medicine)
References